
What Are The Common Changes That Occur With Your Skin When You Are Pregnant?
Around 90% of women experience skin changes during pregnancy. This is hardly surprising considering the huge biochemical and hormonal changes as well as changes to the immune and vascular systems that a woman’s body goes through in the gestational period.
The majority of changes to the skin at this time are harmless, some may be annoying, sore, or upsetting but will not do the mother or baby any real or lasting harm. Symptoms also usually disappear on their own postnatally. However, some skin issues can be an indication of something serious or even potentially fatal.
The following article provides information on some of these skin changes including many of the most common skin-related issues that women face, how to treat them, and when they might be a sign of something less benign.
Disclaimer: This article is for information purposes only. If you have any concerns about skin problems during pregnancy or any other health problems then speak to a medical professional.
How To Treat Pregnancy Stretch Marks Or Striae Gravidarum
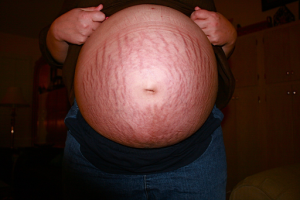
Stretch marks are the most common skin ailment during pregnancy and affect 90% of women in the later stages of pregnancy (the second and third trimesters).
Appearing mostly on the abdomen but also commonly found on the breasts, thighs, and buttocks, these lines are often initially much more vivid in color and can be bright red, pink, purple, brown, or black. They are also slightly indented.
Stretch marks are a slight rupturing of the skin caused by rapid weight gain and/or growth. This is why they appear on the areas of the body which undergo the biggest changes during the antenatal period.
They are totally harmless. Despite being harmless many women find them to be itchy and can also find them upsetting despite them being quite normal and experienced by the majority of women during pregnancy. And by many other people during periods of sudden growth or weight gain which are unrelated to pregnancy – they are common in teenagers for example.
What Can You Do To Reduce The Appearance Of Stretch Marks During Pregnancy?
Many people argue, though the evidence is not conclusive, that improving the elasticity of the skin with good hydration and nutrition will help prevent stretch marks.
This can include drinking plenty of water and eating foods rich in the vitamins, minerals, proteins, and amino acids that help the body to make collagen and hyaluronic acid. These include eggs, fish, chicken, bone broth, capsicums, citrus fruits, garlic, berries, white tea, nuts, and seeds.
There are also plenty of stretch mark-preventing moisturizers, oils, and other skin treatments available to buy. Often these will include ingredients such as cocoa butter, hyaluronic acid, jojoba oil, coconut oil, avocado oil, vitamin e, and vitamin c among others.
Striae gravidarum do not completely disappear although they do usually fade over time and take on a silvery appearance. Creams and oils including moisturizers and retinoids (warning: retinoids are not to be used during pregnancy) may help to reduce the appearance of stretch marks as can cosmetic procedures such as laser treatments and dermabrasion.
Why Does Hyperpigmentation Or Melasma Occur During Pregnancy?
Endocrinological, or hormonal changes during pregnancy, specifically changing levels of estrogen, progesterone, and melanocyte-stimulating hormones (MSH) cause changes in skin pigmentation through increased levels of melanin in between 50 and 90% of all pregnant women.
Most commonly presented as darkening of areola (nipples) which is in itself one of the first signs of pregnancy. Women also often experience darkening of genitals, armpits, and in a line down the middle of their torso, commonly known as the ‘linea nigra’ as their pregnancy progresses.

Between half and three-quarters of women will also notice their moles and freckles becoming darker and will develop dark patches of skin across their cheeks, nose, forehead, and chin – which gives melasma its common name of ‘The Mask of Pregnancy’.
More rarely women may experience more extreme hyperpigmentation with large dark patches. Sometimes these patches completely cover their stomach and breasts for example, but even these extreme cases are harmless and go away naturally postpartum.
How To Treat Hyperpigmentation and Melasma During Pregnancy?
As well as being totally benign it is not possible to prevent this condition. Sometimes the severity, particularly on the face, can be reduced by avoiding exposure to UVA and UVB rays such as avoiding going out in the sun, wearing a sunhat, keeping covered, and wearing a high factor sunscreen. It is also suggested that eating foods rich in folic acid may help reduce hyperpigmentation.
While sunscreen is the best prevention for hyperpigmentation and helps to reduce its progression there are some other ingredients that may help. The first is L-ascorbic acid or vitamin C has been shown to reduce the appearance of pigmentation and is considered to be safe during pregnancy but always consult your doctor before making lifestyle or skincare changes.
The second is retinol or retinoids, this is only for use after pregnancy and breastfeeding. Retinol is often used to help to reduce the appearance of post-pregnancy hyperpigmentation.
What Are Spider Viens or Spider Angiomas?
So named because of the way they look, these harmless, enlarged, visible blood vessels are characterized by one large central blood vessel with smaller off-shooting blood vessels. The central part is the body and the offshoots the legs of the ‘spider’. It is thought that the increased levels of estrogen are the reason why these are so common during pregnancy.
Should You Treat Spider Veins That Occur During Pregnancy?
They disappear with the leveling out of estrogen postpartum and require no treatment. If their appearance is causing distress then they can safely be concealed with makeup.
What You Should Know About Itchy Skin During Pregnancy
Pruritus or itchy skin affects almost all pregnant women at some stage and particularly towards the end of the third-trimester. Itching can have a variety of causes and be surprisingly bothersome, causing stress, discomfort, and lack of sleep. Reasons for itchy skin range from the completely benign:
- Skin stretching to accommodate the growing baby
- Extra weight making itching from the heat more common
- Natural increases in hormone levels
To common and usually harmless skin complaints such as the following:
- Eczema and Dermatitis
- Pruritic Urticarial Papules and Plaques of Pregnancy
- Prurigo of Pregnancy
- Varicose Veins
Eczema and Dermatitis During Pregnancy
Eczema and dermatitis can be itchy, sore and can range from red, dry, scaly, or flaky skin to swelling, lesions, or weeping sores. It can appear anywhere on the body. It is important to know that these symptoms will not harm a growing baby nor will many of the treatments available for these conditions.
Some women find that if they normally experience eczema and/or dermatitis that during their pregnancy it calms down or even disappears. Many other sufferers experience flare-ups either throughout or at particular stages of their pregnancy. Some women who have never had eczema or dermatitis at all previously suddenly develop it at some stage of pregnancy.
Why Does Eczema Flare-up During Pregnancy?
It is thought that changes in chemical balances and hormones are the main cause of developing or changes to the existing condition. There is also the possibility that lifestyle changes, such as diet, environment, medications, and personal products that are brought about by pregnancy may affect existing eczema and dermatitis or trigger it initially.
How To Support Your Eczema During Pregnancy?
Speak to a dermatologist or doctor to see what treatments are suitable. They are likely to recommend emollients (moisturizing lotions, creams, or bathing products). They also might recommend antihistamines or steroid-based creams which are generally considered safe for pregnant women.
What Are Pruritic Urticarial Papules, Plaques of Pregnancy or Polymorphic Eruption of Pregnancy?
Often referred to as PUPPPs or toxic erythema this is the most common pregnancy-specific skin disease and is characterized by a hive-like rash. Despite its worrisome sounding names, it is harmless and usually disappears in the first few weeks postpartum.
Appearing on the abdomen, sometimes within existing stretch marks, and spreading out over the rest of the body over time. This itchy rash usually appears in later pregnancy, in the third trimester.
What Does PUPPPs Look Like?
The rash is usually red in color and slightly raised. It begins as small bumps or papules which then join together creating large plaques. It is thought to be an inflammatory reaction caused by the skin stretching and as such is more common in first pregnancies, multiple pregnancies, and in women who experience excessive or rapid weight gain.
How Will Your Doctor Help Minimize The Symptoms Of PUPPPs?
As other skin problems may appear similar to PUPPPs it is important to seek advice if you have any concerns and to rule out anything more serious.
Treatments include topical over-the-counter remedies such as calamine lotion, or a doctor may prescribe antihistamines or topical corticosteroids.
Itchy Spots Or Prurigo of Pregnancy
Characterized by itchy papules or spots which are often grouped and appear mostly on the limbs and torso prurigo of pregnancy can occur at any time during pregnancy but most often appears in the second and third trimesters.
The small papules often appear red, as they become excoriated due to the itching. Prurigo of pregnancy is not harmful but symptoms can be relieved with emollients (sometimes with menthol), topical corticosteroids, antihistamines, or sometimes phototherapy. It usually disappears on its own postpartum but this can sometimes take weeks or even months.
Does Pregnancy Cause Varicose Veins?
During pregnancy changes in the cardiovascular system, such as an increase in the amount of blood circulating, together with changes in hormone levels which can cause blood vessel walls to relax, often cause varicose veins. Pressure on veins in close proximity to the uterus as it grows can also cause them to become varicose.
They are not usually harmful and often go away following pregnancy however they can be uncomfortable and itchy. The itching is caused by venous statis dermatitis, or blood vessels leaking which can prevent oxygen from reaching the skin. Itching is nothing to worry about. However, if varicose veins are very painful or legs feel sore and heavy it is a good idea to see a doctor to rule out anything more serious such as Deep Vein Thrombosis.
To relieve varicose veins the following often helps:
- Avoid standing for long periods.
- Rest with your feet up.
- Aid circulation with light exercises such as swimming, walking, yoga, and leg exercises.
- Avoid putting on excess weight.
- Gentle massage may help alleviate symptoms.
Sometimes during pregnancy however itching can be a sign of something more serious.
Pemphigoid Gestationis: Rare Auto-Immune Skin Condition During Pregnancy
A relatively rare auto-immune skin disease characterized by itchy blisters which form on the abdomen around the navel usually in the second or third trimesters. The blisters grow and spread throughout the body. It can also be passed onto the baby, who will also get the rash.
Although the rash itself is harmless the blisters do pose a risk of secondary infection. Furthermore, this disease does slightly increase the risk of premature birth.
Treatments are usually in the form of topical corticosteroid creams but antihistamines or oral steroids may even be prescribed.
The rash usually subsides towards the end of pregnancy but can re-emerge during or following the birth or even on resumption of birth control (if hormonal).
Sometimes pemphigoid gestationis is mistaken for PUPPPs which is one reason why it is always important to consult with a doctor about any rashes during pregnancy as a woman with pemphigoid gestationis should be monitored throughout the rest of the pregnancy due to the aforementioned risk.
Intrahepatic Cholestasis of Pregnancy/Obstetric Cholestasis
This is a potentially serious complication of pregnancy that causes the bile acids from your liver, instead of flowing between the liver and the gut, to build up in the body. It can cause premature birth and has also been linked with stillbirths. For these reasons women who suspect they have ICP should speak to their doctor, midwife or obstetrician. They may suggest an early induction (from about 35 weeks) and will probably recommend a hospital birth.
The main symptom of ICP is itching, especially on the hands and feet and that is not accompanied by a rash. There may be other signs such as darker urine, paler feces, and even yellowing of the eyes and skin in some cases. These symptoms can appear at any point during pregnancy but typically ICP appears in the third trimester.
ICP is formerly diagnosed with liver functioning tests.
How To Reduce Pimples During Pregnancy And Why Do They Occur?

Similarly to the acne many teenagers experience due to hormonal changes. The increases in progesterone and androgen during pregnancy, especially in the first and second trimesters, cause many women to experience acne as it causes increased sebum production.
Some women who already experience acne may find it gets worse, others who have never experienced it before may do so. Some people may find that lifestyle and regime changes can help. These include:
- Eating plenty of fresh fruit and vegetables
- Drinking more water
- Cleansing your face twice a day with a mild cleanser. Cleansing more often can cause oil glands to produce more sebum
- Avoided oil-based moisturizers and makeup
- Wash your hair regularly and keep it off your face
- Don’t pick or squeeze pimples
- Avoid touching your face
There are some treatments for acne which may also help. However, it is important to note that some acne treatments must not be used during pregnancy.
Pimple Treatments And Ingredients That Are Safe For Pregnancy
- Products with salicylic acid are thought to be safe to use during pregnancy in concentrations of 2% or less – this is a common ingredient in spot and acne treatments can be found on the shelf.
- Benzoyl Peroxide – often found in over-the-counter acne treatments and is considered safe to use when pregnant. However, it is also recommended that you seek professional advice on safe amounts.
- Hydrocolloidal or treated pimple patches are another great way to minimise the appearance of blemishes. They help to draw out fluid, reducing the size of the pimple and supporting it to heal itself.
Acne Treatments that Must be Avoided when Pregnant
- Retinoids – are a form of vitamin A and usually come in topical creams or gels. They are effective against acne. However, the use of these retinoids during pregnancy can cause birth defects.
- Isotretinoin – This is a very effective medication for acne that is taken orally and is a form of retinoid. It carries a very high risk of causing severe and potentially fatal birth defects. Doctors will only prescribe to women of childbearing age if they are using 2 forms of contraception and take monthly pregnancy tests.
- Hormone therapy – This is sometimes an effective acne treatment. Estrogen and anti-androgens are commonly used. However, they are avoided during pregnancy as they can cause birth defects.
- Oral Tetracyclines and Antibiotics – studies have shown that these prescription medications may cause bone and teeth problems in developing babies.
Always seek medical advice for skin or other health related problems or before treating skin issues especially during pregnancy.
References:
Beard MP, Millington GW. Recent developments in the specific dermatoses of pregnancy. Clin Exp Dermatol. 2012 Jan;37(1):1-4; quiz 5. doi: 10.1111/j.1365-2230.2011.04173.x. Epub 2011 Oct 18. PMID: 22007708.
Bolanca I, Bolanca Z, Kuna K, Vuković A, Tuckar N, Herman R, Grubisić G. Chloasma–the mask of pregnancy. Coll Antropol. 2008 Oct;32 Suppl 2:139-41. PMID: 19140277.
Kar S, Krishnan A, Shivkumar PV. Pregnancy and skin. J Obstet Gynaecol India. 2012 Jun;62(3):268-75. doi: 10.1007/s13224-012-0179-z. Epub 2012 Aug 28. PMID: 23730028; PMCID: PMC3444563.
Kroumpouzos G, Cohen LM. Dermatoses of pregnancy. J Am Acad Dermatol. 2001 Jul;45(1):1-19; quiz 19-22. doi: 10.1067/mjd.2001.114595. PMID: 11423829.

