People with diabetes have a higher risk of skin problems and complications that arise from them. Skin problems can also be a warning sign for pre-diabetes or a symptom of undiagnosed diabetes. This guide will cover what diabetes is and why it affects the skin as well as common dermatological problems associated with diabetes, and potential treatments. It will also provide an overview of skin symptoms that may be indicative of diabetes and should be followed up with a doctor.
What is Diabetes?
Type 1 Diabetes
In people with type 1 diabetes, the body cannot naturally make the hormone insulin. Insulin is essential because its job in the human body is to allow glucose into the body’s cells to fuel them. Without insulin, the glucose that we get from carbohydrates in food and drinks cannot enter the body’s cells and so stays in the bloodstream causing high blood sugar levels which lead to the symptoms associated with diabetes: extreme tiredness, extreme hunger, and thirst, frequent urination. Diabetes can also put immense stress on the rest of the body’s systems including the cardiovascular system and organs such as the kidneys and liver.
Nobody is entirely sure what causes Type 1 diabetes but it is not related to lifestyle choices including diet. People with Type 1 diabetes have to take insulin to live and will also have to help manage the condition with careful eating and planning of day-to-day activities.
Type 2 Diabetes
Type 2 diabetes is the more common type of diabetes. Approximately 90% of people who have diabetes have type 2. With type 2 diabetes although the pancreas does produce insulin, the insulin does not work well enough, so the blood sugar level increases and prompts the production of more insulin – if untreated this overwork can cause the pancreas to stop working completely. Type 2 can be more difficult to spot because the symptoms can develop gradually. It also does have known factors that can make it more likely that someone will develop type 2 diabetes; these include being overweight or obese and if family members have had a diagnosis.
Gestational Diabetes
This form of diabetes occurs in pregnant women. It is most common within the 2nd and 3rd trimesters of pregnancy. In many countries; the UK and USA included women are screened for gestational diabetes as a matter of course because it is so common. Some factors make it more likely that women will develop diabetes during pregnancy these are:
- being overweight
- a gestational diabetes diagnosis in a previous pregnancy
- a close family member (parent or sibling) with a diabetes diagnosis
- Black, Asian, African-Caribbean, or Middle-Eastern heritage
- delivered a large baby (over 10lbs or 4.5kg) previously
It is important women are screened for gestational diabetes especially those in higher-risk categories. This is in part because symptoms of gestational diabetes are similar to symptoms often associated with the pregnancy itself such as:
- tiredness
- urinating more frequently
- increased thirst
Gestational diabetes can cause complications including premature labor and birth, pre-eclampsia, jaundice in the newborn, and very rare cases can cause the loss of the baby. It also puts the mother in a higher risk group for developing type 2 diabetes at a later stage.
Why Does Diabetes Affect Skin?
The increased levels of glucose in the bloodstream can lead to fluid loss. One of the symptoms of diabetes is increased urination, as the body tries to rid itself of sugar. The lowered levels of fluid in the body mean that dry skin is common among diabetic patients, particularly on the legs, elbows, and feet. When skin is dry it is likely to become cracked and cracked skin can more readily become infected. This is compounded by the fact that another side effect of having higher levels of sugar in the blood is a decreased ability for white blood cells to stave off infections.
As well as an increased risk of infection diabetes can also slow the body’s ability to heal from infections and wounds. This can lead to additional complications and skin complaints.
What Skin Problems are Associated with Diabetes
The increase in blood sugar levels, particularly in poorly managed or undiagnosed diabetes, can increase the likelihood of a variety of skin problems. Other skin problems are associated with diabetes either for reasons unknown or due to the variety of complications that occur from this disease. It is estimated that 30% of people with diabetes will have at least one occurrence of diabetes-related skin problems. For some skin disorders and some groups of diabetics the likelihood is dramatically increased – see information on some of the different related skin disorders for more details.
Diabetes-Related Skin Problems Include:
- Psoriasis
- Impetigo
- Vitiligo
- Candida intertrigo
- Diabetic Stiff Skin
- Diabetic dermopathy
- Diabetic bullae
- Scleroedema
- Foot Ulcers
- Pruritus
- Necrobiosis lipoidica
- Granuloma Annulare
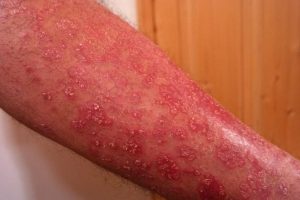
Psoriasis
Those with type 2 diabetes are twice as likely as people without diabetes to have psoriasis. Researchers believe this may be due to genetic factors. Those with psoriasis should be extra vigilant regarding screening for diabetes and consulting a doctor if they are showing any other symptoms. Characterized by dry, red skin with white or silver scales, psoriasis is an immune response that causes the body to over-produce skin cells. It can appear anywhere on the body but is most commonly found on knees, elbows, and scalp. Psoriasis can be itchy and sore.
It tends to come and go and can often be cyclical. Treatments include, for mild to moderate psoriasis emollient and/or steroid-based creams to light therapy and oral/injected medications for more severe cases. Sometimes these treatments work best in conjunction with one another and every person will need individualized treatment as what works for one person will not necessarily work for another.
Impetigo
Skin infections such as impetigo are more common in people with diabetes. Impetigo is a common bacterial infection of the skin which causes blisters and pustules which quickly burst and scab over leaving golden-colored scales. They are often small and usually occur around the nose and mouth but can also appear on the trunk or around the genital area. It can also spread to larger areas if left untreated and is highly contagious. With treatment, which is either a topical or oral antibiotic, impetigo clears up after about a week. Left untreated it will get better but will take longer. As well as the blisters and plaques some people may experience a general feeling of being unwell, tiredness, and sometimes a fever.

Vitiligo
Often associated with autoimmune diseases including adult-onset type 1 diabetes Vitiligo is thought by researchers to be a form of autoimmune disease itself. It is characterized by patches of un-pigmented skin due to the destruction of the specialist skin cells which contain pigment, called melanocytes.
Vitiligo can be found anywhere on the body and can also affect hair color including eyelashes and eyebrows. Sometimes it affects relatively small areas of the body or sometimes it more widespread. Vitiligo is not painful, nor does it cause any other problems other than making skin more sensitive to the sun so those affected should ensure to wear adequate sunscreen and cover-up. However, it can cause people embarrassment and anxiety.
Candida intertrigo
Candida refers to a fungal infection. Intertrigo means inflammation of skin folds. Therefore the two together combine to make a fungal infection in areas of the body where there are skin folds typically, the vagina, scrotum and buttocks, armpits, between the fingers and toes, and areas where excess body fat creates folds such as the abdomen or underneath the breast tissue. Candida intertrigo is characterized by raw, red, itchy, and sometimes oozing skin which can have a foul smell as well. The skin may also crack and therefore be at increased risk of bacterial infection. Triggers and causes include lack of air circulation, heat, moisture, friction, and contact with urine, feces, or sweat. People with diabetes, especially those whose blood sugar levels are poorly managed are at increased risk of candida intertrigo because of the increased glucose in the blood. The candida bacteria feeds on sugar so this combined with the warm, moist environments provided by skin folds creates a perfect environment for this bacteria to grow. To help prevent this skin problem it is important to get the blood glucose levels under control with diet and/or insulin. Those who are overweight or obese will naturally have more environments in which the candida intertrigo will develop and grow so maintaining or attaining a healthy weight is advised. Other prevention tips include keeping skin folds clean and ensure they are dry, using talcum powder, and wearing loose, cotton clothes. Treatments are using either topical antifungal creams such as clotrimazole or in more severe cases itraconazole or fluconazole which are oral antifungal treatments.
Diabetic Stiff Skin
For those with type 1 diabetes, a complication that they often suffer from, particularly in long-standing cases is digital sclerosis, also known as diabetic stiff skin. It affects around one-third of those with type 1 diabetes. Digital sclerosis is thought to be caused by reactions between proteins in the skin combining with glucose which creates an increase in glycation end products. The symptoms of diabetic stiff skin are thickened, waxy, yellow skin forming on the hands leading to lessened mobility of the hand and joints. There is no treatment other than effective management of type 1 diabetes.
Diabetic Dermopathy
Occurring in around 1/3 of people with diabetes, the skin condition Diabetic dermopathy appears as round or oval patches which are red or light brown. Appearing most often in older patients or those who have had diabetes for over 10 years the patches are usually initially scaly and later indented. Due to these patches often appearing on the shins diabetic dermopathy is also commonly known as shin spots but may also be referred to as pigmented pretibial patches. There is no treatment available for this skin complaint other than better management of blood sugar levels. They are not harmful and neither do they cause pain or discomfort.
Diabetic bullae
Also called bullosis diabecticorum these are often large, irregularly shaped blisters. They can range from half a centimeter to up to nearly 20cm in size but are mostly painless and appear spontaneously. Thankfully this complication of diabetes is rare and the blisters heal by themselves, especially if the blisters remain unbroken. If blisters do break patients must be extra vigilant for signs of infection.
Scleroedema
This is a rare skin disorder, the cause of which is unknown. However, it is associated with type 2 diabetes as well as immune disorders such as rheumatoid arthritis and other diseases. Sclerodema is characterized by thickened, hard skin with an orange-peel-like texture. The affected areas can also be brownish or red. There are 3 types of sclerodema but it is type 3 that is mostly associated with diabetes, it is also called scleroedema diabeticorum and occurs over the neck and upper back.
Foot Ulcers
Often starting as a subepidermal blister which leads to a small, circular, indented skin sore which, in turn, can spread to a large full-thickness sore. Diabetic foot ulcers are often painless, this is one of the reasons why they are often presented to medical professionals late and commonly become infected. Infections can become very serious as they can lead to complications such as gangrene, cellulitis, or osteomyelitis (bone infection). Diabetic patients with type 2 diabetes are more prone to foot ulcers and those who have had diabetes for over 10 years. It is also more common among male patients. Foot ulcers are related to the neuropathy or loss of feeling which is often a result of high blood glucose levels especially over extended periods, this is simply because the pain that would usually signal a change in position, footwear, or alert the patient to an injury does not occur.
Pruritus
Pruritus essentially means itchy skin and is associated with diabetes for varying reasons. Itching is often a symptom of many of the other skin conditions listed which can occur are associated with diabetes including dry skin, psoriasis, and candida intertrigo. It is also a symptom of nerve damage or neuropathy which diabetes can cause.
Diabetics are more likely to have high levels of cytokines in the body – the presence of these proteins are known to cause inflammation, which in turn can cause itching. Far from being the insignificant problem those who haven’t experienced it might assume pruritus can not only be uncomfortable but can lead to anxiety and depression, insomnia. Furthermore, the scratching that naturally follows can cause pain as well as secondary and more serious complications such as infections. Not only can the itching and scratching that follows be worrisome but it can also be an indication of other associated problems including kidney or liver failure.
Therefore those with diabetes must speak to a doctor about any pruritus they experience.
Preventing itchiness strategies can include effective management of blood sugar levels, wearing loose, cotton clothes, adequate hydration, and avoiding perfumed skin products. Treatments include fragrance-free or hypoallergenic moisturizers and treating the cause of the itching.
Necrobiosis Lipoidica
Affecting the shin areas of diabetics who are insulin-dependent (and rarely non-diabetics too) necrobiosis lipoidica is an inflammatory skin disorder of unknown cause. It is more common among women and in those who are obese or who have thyroid problems or disease or hypertension. Necrobiosis Lipoidica is characterized by scaly brown or yellow patches usually oval in shape and with shiny centers. The skin in the patch thins over time which can lead to injuries prone to bacterial infection and/or take a long time to heal. Mild cases may require no treatment at all and should just be monitored for escalation/secondary infection. More severe cases may be treated with a range of treatments including localized steroids, antibiotics, targeted biological therapies, or UV radiation/phototherapy/psoralens-UVA therapy.
Granuloma Annulare
Occurring in around 4% of people with diabetes and more common in women this usually asymptomatic skin rash appears as clearly defined rings or arcs that are up to around 5cm in diameter. Often raised and red but also can be brown or skin-colored there can be a few marks often only appearing on the hands and/or feet, or they can appear all over the body. It is in more widespread cases that Granuloma Annulare becomes symptomatic usually with itching. Sometimes this rash is triggered by high levels of glucose in the blood but can also be triggered by allergic reactions to medication, insect bites, vaccinations, injuries, or as a symptom of a disease such as hepatitis. Granuloma usually requires no treatment and will go away by itself after a maximum of around 2 years. However, if symptoms are causing problems or there are other health concerns a doctor should be consulted and might prescribe a topical cream.
Disclaimer
Information in this article is not a substitute for medical diagnosis and treatment. Always seek advice of a professional if you have any health concerns including any of the skin complaints mentioned above.
References:
George, Susannah.MC. and Walton, Shernaz. British Journal of Diabetes, Vol. 16, Issue 2. pp58- 61. April/June 2016.
Paron, Nicholas. G and Lambert, Philip. W. Cutaneous Manifestations of diabetes mellitus. Primary Care, 27 (2), pp371-383. 2000.
www.aad.org
www.dermnetnz.org
www.diabetes.org.uk
www.diabetes.org/diabetes/complications/skin-complications
www.psoriasis-association.org.uk

